2 AM in a Rural Emergency Room
It is 2 AM at a 25-bed critical access hospital in eastern Montana. A 58-year-old rancher arrives in the emergency department with sharp chest pain and shortness of breath. The attending physician orders a chest X-ray. The portable unit produces the image within minutes. But now the image sits on a screen, and there is no radiologist within 90 miles.
The ER doctor is experienced. She can read a straightforward fracture or an obvious pneumothorax. But this film is ambiguous — there is something in the left lower lobe that could be an infiltrate, could be atelectasis, could be the early signs of something more concerning. She needs a specialist’s eyes, and she needs them now, not when the locum radiologist arrives for Tuesday’s clinic.
This scenario plays out thousands of times every week across rural America. It is not a failure of effort or dedication. It is a structural problem — one that teleradiology began to address years ago, and one that AI is now positioned to help solve in a meaningful way.
The Rural Radiology Crisis by the Numbers
The scale of the diagnostic gap in rural healthcare is significant and well-documented.
Approximately 60 million Americans live in areas designated as Health Professional Shortage Areas for radiology. According to the Association of American Medical Colleges, the United States faces a projected shortage of up to 42,000 specialists by 2033, and radiology is among the specialties most affected. Rural areas bear a disproportionate share of that shortage.
Consider the geography. There are roughly 1,800 rural hospitals in the United States. Many of these facilities serve as the sole source of emergency and diagnostic care for communities spread across vast distances. In states like Wyoming, Montana, and the Dakotas, patients may live two or more hours from the nearest hospital with full-time radiology coverage.
The consequences are measurable. Studies published in the Journal of the American College of Radiology have shown that patients at rural hospitals experience longer turnaround times for radiology reads — sometimes 4 to 12 hours for non-emergent studies, and even critical findings can face delays when coverage is limited to daytime hours. Delayed diagnoses lead to delayed treatment. For time-sensitive conditions like stroke, pulmonary embolism, or tension pneumothorax, those delays can directly affect survival.
Rural hospitals also face a recruitment challenge that compounds the shortage. Fewer than 4% of practicing radiologists work in rural settings. Competitive salaries, urban lifestyle preferences, and the professional isolation of solo practice make it difficult to attract and retain specialists. Even facilities that manage to recruit a radiologist often depend on a single practitioner who cannot provide around-the-clock coverage.
The gap is not just about convenience. It is about clinical outcomes, patient safety, and the fundamental question of whether geography should determine the quality of care a person receives.
What Teleradiology Solved — and What It Didn’t
Teleradiology emerged as a practical response to the rural radiology shortage, and it has delivered real benefits. By transmitting medical images electronically to off-site radiologists, teleradiology allowed rural hospitals to access specialist reads without requiring a radiologist on the premises.
The impact has been substantial. Teleradiology services now support a large share of rural hospital radiology workflows. Nighthawk and daytime remote reading services have given small facilities access to board-certified radiologists they could never have recruited locally. For many rural emergency departments, teleradiology transformed the standard of care.
But teleradiology has limitations that have become more apparent over time.
Coverage gaps persist. Even with teleradiology contracts, many rural hospitals face periods — late nights, weekends, holidays — where turnaround times stretch. Remote reading services manage their own workloads, and a single teleradiologist may be covering dozens of facilities simultaneously. Priority is triaged, but delays are inherent.
Cost pressures are real. Per-read teleradiology fees add up, particularly for small hospitals operating on thin margins. Critical access hospitals — the financial backbone of rural healthcare — often run at break-even or a loss. Every additional cost is scrutinized, and some facilities limit teleradiology use to emergencies only, leaving routine studies to wait.
The sharing problem remains. Traditional teleradiology depends on established relationships between a hospital and a reading service. But what happens when a rural clinic — not a hospital — captures an image and needs to get it to a specialist quickly? Or when a patient needs a subspecialist opinion that the contracted teleradiology group cannot provide? The infrastructure for ad hoc, frictionless image sharing has historically been lacking.
No immediate triage layer exists. When a study is sent to a teleradiology service, it enters a queue. There is no mechanism to provide the ordering physician with an immediate preliminary assessment while the full read is pending. For the ER doctor at 2 AM, the wait between sending the image and receiving the interpretation is a period of clinical uncertainty.
Teleradiology addressed the most critical piece of the puzzle — getting specialist eyes on rural images. But it left gaps in immediacy, flexibility, and cost-efficiency that the next generation of tools needs to fill.

AI as the Always-On First Pass
This is where AI-assisted radiology enters the picture — not as a replacement for radiologists, but as a layer of immediate, always-available support.
MYAIRA AI functions as an AI second reader for radiological studies. It analyzes chest X-rays and detects more than 15 pathologies, including pneumothorax, pleural effusion, cardiomegaly, consolidation, mass lesions, and rib fractures. When it identifies urgent findings, it flags them for priority triage, giving clinicians an immediate signal that a study requires urgent attention.
For rural hospitals, the value proposition is straightforward. The AI does not sleep, does not take holidays, and does not manage a queue of studies from 30 other facilities. When an image is captured, MYAIRA AI can process it and return a preliminary analysis within moments.
To be clear about what this is and what it is not: AI second reads are decision support, not definitive diagnoses. They do not replace the radiologist’s interpretation. What they provide is an immediate layer of clinical intelligence that helps the ordering physician prioritize and act while the formal read is in progress.
In our rural ER scenario, this changes the clinical workflow meaningfully. The ER physician orders the chest X-ray. Within moments of the image being captured, MYAIRA AI analyzes it and flags a finding consistent with a left lower lobe consolidation with possible effusion. The physician now has a data point — not a final diagnosis, but an informed signal — that supports her clinical suspicion and helps guide her next steps. She can begin treatment protocols while the teleradiology read is pending, rather than waiting in uncertainty.
For facilities with limited overnight coverage, this kind of immediate AI triage can be the difference between early intervention and hours of watchful waiting.
Instant Sharing Bridges the Last Mile
The other gap that technology needs to address is the sharing problem. Rural clinics and small hospitals often lack the PACS infrastructure, VPN connections, or institutional relationships needed to share images quickly with specialists outside their immediate network.
Medixshare, MYAIRA’s scan-sharing platform, is designed to solve this specific problem. It enables any facility — including small clinics with no special infrastructure — to share medical images instantly with any specialist, anywhere. There is no requirement for both parties to be on the same PACS system, no need for complex IT setup, and no dependency on pre-existing teleradiology contracts.
This matters for rural healthcare in several concrete ways.
Subspecialty access. A rural hospital’s teleradiology contract may cover general radiology reads competently. But when a study needs a neuroradiology or pediatric radiology opinion, the contracted group may not have that expertise. Medixshare allows the facility to reach the right specialist for the specific clinical question, on demand.
Clinic-to-specialist pathways. Not all imaging happens in hospitals. Rural primary care clinics, urgent care facilities, and outpatient imaging centers also capture studies that need specialist review. Medixshare gives these smaller facilities a direct path to expert interpretation without requiring hospital-grade infrastructure.
Referral coordination. When a rural facility identifies a finding that requires transfer to a tertiary center, the ability to share imaging instantly with the receiving facility’s specialists accelerates the transfer process. The receiving team can review the images before the patient arrives, enabling them to prepare and reducing the time from arrival to treatment.
No infrastructure barriers. Many rural facilities operate on aging IT systems with limited bandwidth and minimal technical staff. Medixshare is designed to work within these constraints — no special hardware, no complex integration requirements, no dedicated IT support needed to get started.

The Combined Workflow: AI Plus Sharing
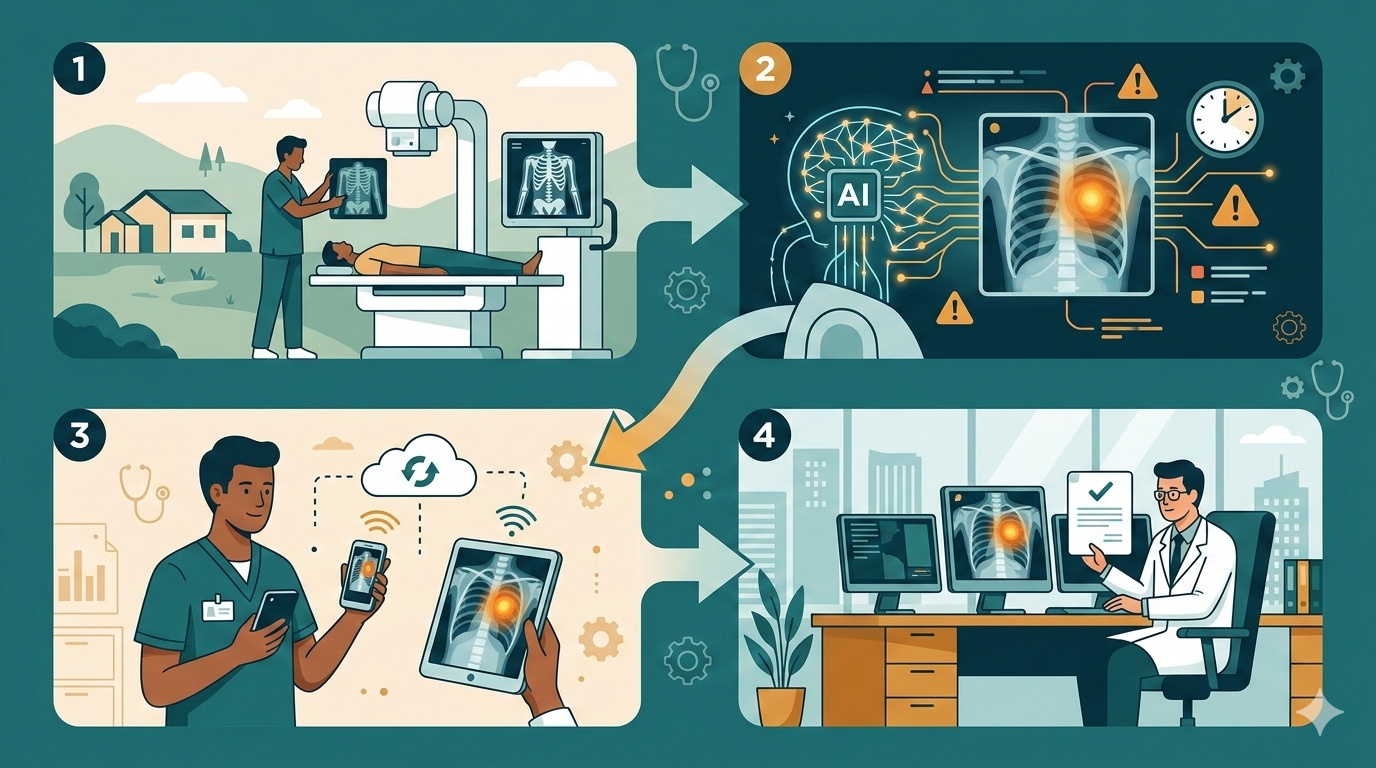
The real power of these tools emerges when they work together. Consider the complete workflow for a rural facility using both MYAIRA AI and Medixshare.
A patient presents at a rural clinic. The clinician orders imaging. The study is captured on the facility’s existing equipment.
Step one: Immediate AI analysis. MYAIRA AI processes the image and returns a preliminary analysis. If urgent findings are detected — a pneumothorax, a large effusion, a suspicious mass — the system flags them immediately. The clinician receives this information within moments of the image being captured.
Step two: Informed clinical decision-making. Armed with the AI’s preliminary findings, the clinician can begin appropriate clinical responses. If the AI flags a tension pneumothorax, the clinician does not need to wait for a teleradiology read to begin emergency intervention.
Step three: Instant specialist sharing. Simultaneously, the clinician uses Medixshare to share the study with a remote radiologist or subspecialist for a definitive read. The specialist receives the images instantly, along with the AI’s preliminary findings, providing context that helps prioritize the read.
Step four: Formal interpretation. The remote specialist provides the official read. Because the AI has already flagged the urgent findings and the images were shared instantly, the time from image capture to formal interpretation is compressed significantly compared to traditional teleradiology workflows.
This combined approach does not eliminate the need for teleradiology services or specialist radiologists. It makes the entire system work better — faster triage, shorter wait times, and fewer moments where a clinician is making decisions in an information vacuum.
For facilities on MYAIRA’s Enterprise plan, this workflow integrates directly with existing PACS systems. The AI analysis runs automatically on incoming studies, flagging results within the existing clinical workflow. Unlimited AI analyses mean there is no per-study cost calculation to discourage use. And on-premise or private cloud deployment options address the data security and compliance requirements that hospital IT departments rightly prioritize.
What This Means for Patients
The technology matters only insofar as it changes outcomes for patients. In rural healthcare, those potential changes are significant.
Faster time to diagnosis. When AI provides immediate preliminary findings and images can be shared instantly with specialists, the interval between imaging and actionable information shrinks from hours to minutes. For conditions where time is a clinical factor — stroke, PE, aortic dissection — this compression can be life-altering.
Fewer unnecessary transfers. Rural hospitals transfer patients to urban centers when they lack the diagnostic confidence to manage a case locally. Some of those transfers are medically necessary. But some are driven by diagnostic uncertainty — the inability to get a timely specialist read. When AI triage and instant specialist access reduce that uncertainty, some transfers become unnecessary. The patient stays closer to home, closer to family, and avoids the physical and financial burden of a long-distance transfer.
More equitable care. The fundamental promise of these tools is simple: a patient’s access to diagnostic expertise should not be determined by their zip code. A rancher in eastern Montana and a resident of downtown Chicago should both have access to timely, accurate radiology reads. We are not there yet, but the combination of teleradiology, AI-assisted triage, and frictionless image sharing is closing the distance.
Clinician support and retention. Rural clinicians carry an enormous burden. They make high-stakes decisions with fewer resources and less specialist support than their urban counterparts. Tools that reduce clinical uncertainty and provide immediate decision support are not just good for patients — they reduce the isolation and stress that drive rural clinician burnout and attrition.
The Road Ahead
The diagnostic gap in rural healthcare was not created by a single cause, and it will not be closed by a single solution. Workforce development, reimbursement reform, broadband expansion, and policy changes all have roles to play.
But technology can make a material difference today. AI-assisted second reads provide the immediate triage layer that rural clinicians need during off-hours and coverage gaps. Instant scan sharing through tools like Medixshare breaks down the infrastructure barriers that have kept small facilities isolated from specialist expertise. Together, they create a more responsive, more accessible diagnostic ecosystem for underserved communities — and it is this kind of impact that drives AI Bharata’s mission to make diagnostic AI accessible regardless of geography or facility size.
The 2 AM chest X-ray in rural Montana does not have to be a moment of clinical uncertainty. With the right tools, it can be a moment where technology ensures that distance does not dictate the quality of care.
Watch: How teleradiology and AI bridge the rural diagnostic gap
Interested in bringing AI-assisted radiology and instant scan sharing to your facility? Learn about MYAIRA for hospitals and discover how our platform supports rural and critical access hospitals with the diagnostic tools their communities deserve.
